Publications

Physically Active Adults with Low Back Pain do not Demonstrate Altered Deadlift Mechanics: A Novel Application of Myotonometry to Estimate Inter-Muscular Load Sharing
Authors: Jared M. McGowen 1, Stephanie R. Albin 2, Carrie W. Hoppes 3, Jeffrey S. Forsse 1, John Abt 4, Shane L. Koppenhaver 5
Affiliations:
- Health, Human Performance, and Recreation, Baylor University
- School of Physical Therapy, Regis University
- Army-Baylor University Doctoral
- Program in Physical Therapy, Baylor University
- Children’s Health Andrews Institute for Orthopaedics and Sports Medicine
- Doctoral Program in Physical Therapy, Baylor University
Journal: International Journal of Sports Physical Therapy - January 2024, Volume 19, Issue 1, Pages 1462-1472 (DOI: 10.26603/001c.90707)
-
Field & Applications:
- Medical
- Sport
- Musculoskeletal disorder
- Low back pain
- Muscle development / Performance
- Recovery from injury
- These findings contribute to the growing body of literature regarding how muscle stiffness relates to LBP and how myotonometry may be used to monitor for neuromuscular deficits that have been difficult to reliably quantify with other clinical methods.
Background: Rehabilitation clinicians that work with physically active populations are challenged with how to safely return patients back to performing deadlift movements following low back injury. Application of reliable and valid tests and measures to quantify impairments related to low back pain (LBP) enhances clinical decision making and may affect outcomes. Myotonometry is a non-invasive method to assess muscle stiffness which has demonstrated significant associations with physical performance and musculoskeletal injury.
Hypothesis/Purpose: The purpose of this study was to compare the stiffness of trunk (lumbar multifidus [LM] and longissimus thoracis [LT]) and lower extremity (vastus lateralis [VL] and biceps femoris [BF]) muscles between individuals with and without LBP during the lying, standing, and deadlifting body positions.
Study Design: Cross-sectional cohort comparison.
Methods: Muscle stiffness measures were collected in the VL, BF, LM, and LT muscles with participants in lying (supine and prone), standing, and the trap bar deadlift position. Separate analyses of covariance were conducted to compare absolute and relative muscle stiffness between the groups for each muscle and condition.
Results: Sixty-eight participants (41 female, 21.3 years, 34 LBP) volunteered for the study. Within the deadlift condition there was a significantly greater increase in the percent-muscle stiffness change in the VL (p = .029, 21.9%) and BF (p = .024, 11.2%) muscles in the control group than in the LBP group. There were no differences in percent-muscle stiffness changes for the standing condition nor were there any absolute muscle stiffness differences between the two groups for the three conditions.
Conclusion: No differences in muscle stiffness were identified in the lying, standing, or deadlifting conditions between participants with and without LBP. Differences in percent stiffness changes were noted between groups for the deadlift position, however the differences were modest and within measurement error. Future studies should investigate the utility of myotonometry as a method to identify LBP-related impairments that contribute to chronic and/or recurrent low back injury.
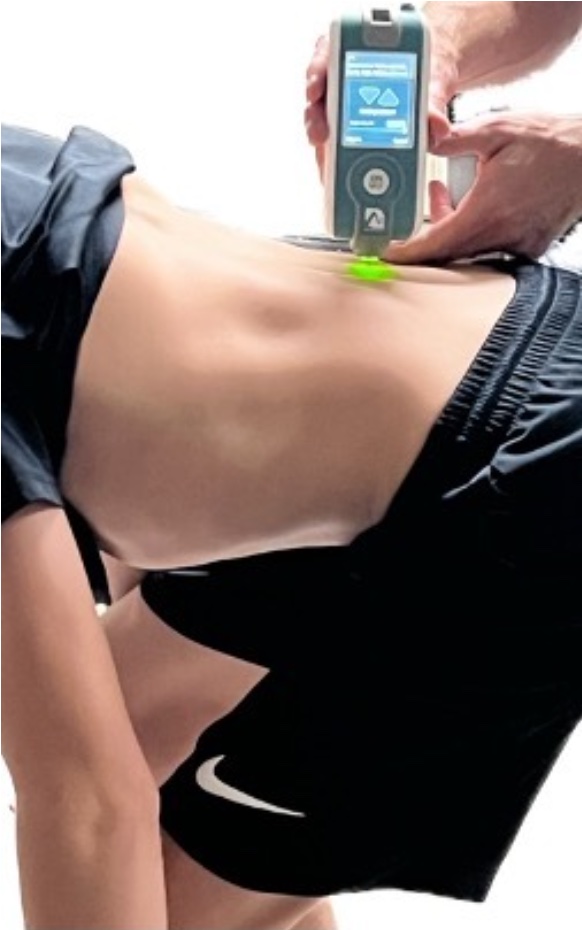
Figure 2. Obtaining stiffness measure of the lumbar multifidus muscle with the MyotonPRO.
Keywords: muscle stiffness, neuromuscular function, rehabilitation, clinical decision making
The results of this study indicate that no significant differences in muscle stiffness exist between participants with LBP and healthy controls in the lying, standing, or deadlifting conditions. Although differences in percent-muscle stiffness changes were noted between groups for the deadlift position, the differences were within measurement error. Future studies should seek to expand on these findings by using myotonometry to further investigate the relationships between muscle stiffness and deadlift performance in LBP populations of varying degrees of pain and/or disability.


